Neurodivergents
and Autism
(¯`*•.¸,¤°´✿.。.:* 𝚰𐓣𝖼𝗋𝖾ᑯ𝗂ᑲᥣ𝖾𝐇ⱺ𝗋𝗂ƶⱺ𐓣𝗌.ⱺ𝗋𝗀 *.:。.✿`°¤,¸.•*´¯)

In a flower garden the water and nutrients in the soil combine to allow the seeds to germinate, then the sun comes in so the stems will be sturdy enough to hold our beautiful blooms.
Just like in Autism, the biomedical approach will allow the gut and nervous system to heal for germination... only then can a integrative treatment plan can be strengthened
and joy and success can be enjoyed...
and your children can flourish...(or bloom).
What is Autism?
Yet one out of forty of their clients have Autism of one type or another.
Misconceptions about autism are prevelent in todays America and around the world in society and in the medical profession. So it is crutial that both the medical professions and our citizens become aware of the following research and information on Autism.
It is a growing field and the more that we learn the more we realise that this is more prevelant now, than ever before.
(LIKE IN THE BIOMEDICAL INTEGRATIVE MODEL AND THE NEURODIVERSITY APPROACH)
LINKS GO TO THE ACTUAL MEDICAL RESEARCH
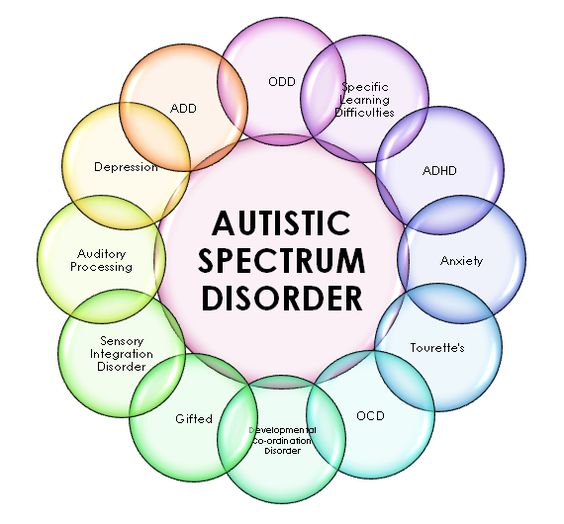
For example, hyperlexia can have ten other diagnosises depending on what type of professional that you met with. Here are 10+ common diagnoses a hyperlexic child might also have (besides autism). ADHD is the same way.

Autism is like a bouquet of flowers:
they both have many varieties and combinations.
When we can treat them at the roots, they can flourish.
Medical doctors simply haven't had the experiences, and the training to diagnose it, no less treat it. Everyone seems to have an image of what it looks like in a nieghbor, a family member, or even a friend or their children. Doctors try to make sense of alot of sensory, psychological, digestive and physical anomalies that seem linked to other illnesses. So they miss the diagnosis of autism and assgn a few of the symptoms to something they are familiar with. So this is really a huge problem that medical professionals have yet to take on. Left untreated as a whole diagnosis, is detrimental to ones development and can lead to:
Problems with social interactions, communication and behavior
Problems in school and with successful learning
Employment problems
Inability to live independently
Social isolation
Stress within the family
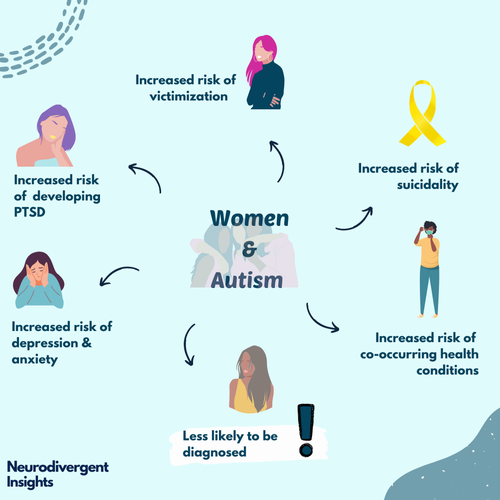
Victimization and being bullied
The disorder also includes limited and repetitive patterns of behavior. The term "spectrum" in autism spectrum disorder refers to the wide range of symptoms and severity.
Autism spectrum disorder includes conditions that were previously considered separate — autism, Asperger's syndrome, childhood disintegrative disorder and an unspecified form of pervasive developmental disorder. Some people still use the term "Asperger's syndrome," which is generally thought to be at the mild end of autism spectrum disorder.
While there is no cure for autism spectrum disorder, intensive, early treatment can make a big difference in the lives of many children.
For More information See The Mayo Clinic's Autism Pages
Professionals CLICK HERE for Rossignol Medical Center
Am I autistic?
Many of us at Autistic Parents only discovered we are autistic in adulthood, often after our children were identified. We frequently get contacted by parents who are currently going through this process and, although our main focus is providing peer support for parents who positively identify as autistic (including self-diagnosis), we’ve created this blog post to signpost anyone who finds themselves in this situation to helpful resources.
If your child is the first one in the family to be identified as autistic it can be surprising and confusing. You may not have realised there was anything unusual about your child’s behaviour because you did those things when you were little. It can be a surprise to realise things that are normal for you, are actually autistic traits. Maybe you see your child struggling and you can relate to them more easily than others, because you struggle in similar ways.
This then leads you to question: Am I autistic?
What is Autism?
The first thing you need to understand is that everything you think you know about autism is probably wrong.
Currently, there is no scientific consensus on what autism actually is. There is no blood test or brain scan that can identify an autistic person. The medical definition of autism, as found in diagnostic manuals, is based on observations of autistic people and how they behave when they are stressed. Discussions around autism have been dominated by non-autistic professionals and parents, which has created a very negative view. Mainstream knowledge about autism is based on outdated stereotypes.
Today, thanks to the work of autistic adults who have shared their lived experience, we have much more information and understanding of what being autistic actually means. We know that autism is not an illness or tragedy, it’s just a difference in the way someone experiences the world and communicates with others.
Autism Epidemic?
Rates of autism diagnosis have drastically increased in recent years. This is not because there are more autistic people than there used to be, it’s simply due to the fact that medical professionals are slowly getting better at identifying us. The most recent diagnostic criteria for autism were published in 2013. Professionals have also started to realise that girls and women can be autistic too. These factors mean that many people who would have been missed in childhood are now getting diagnosed as adults.
Heritability of Autism
We know that autism has genetic factors and tends to run in families. A 2017 study showed the heritability of autism to be 83%. A family history of autism means you are more likely to be autistic yourself. If you have a child diagnosed as autistic, there’s a high probability that you are too.
Online Tests
There are many online tests for autism that can seem appealing because they are quick and seem to offer an easy answer. If you decide to take online tests or quizzes, be aware that these tests are generally created by non-autistic people and are often based on stereotypes of autism, such as being obsessed with trains or being brilliant at maths. Some of the questions can also be ambiguous and open to interpretation. While they can be helpful to get an idea of whether you have some autistic traits, you can score highly on a test and not be autistic, and you can also score low on a test and still be autistic. They can’t tell you for definite whether you are autistic.
Autistic Lived Experiences
What can be more helpful is learning about the experiences of other autistic adults, and seeing if they resonate with you. These stories share what it actually feels like to be autistic, rather than what it looks like to non-autistics. Following the #ActuallyAutistic hashtag on social media is a great way to start connecting with and learning from people who are autistic themselves. There are also many online groups for people who are exploring whether they could be autistic, as well as blogs, vlogs, podcasts, and books based on lived experience.
Formal Diagnosis
If you have been thinking about whether you could be autistic for a long time, you may be considering whether to go through the assessment process to get a formal diagnosis. Whether you decide to pursue this or not is entirely up to you. There are pros and cons to getting a formal diagnosis and there are barriers to getting a diagnosis which may make it more difficult for some people. At Autistic Parents UK we feel that self-diagnosis is valid. If you positively identify as autistic and you are a parent in the UK you are welcome to access any of our peer support services.
Resources to Explore
Here are some resources our volunteers at Autistic Parents UK found helpful when they were exploring whether they may be autistic. These links contain a wealth of information and are all created by autistic people. Whether you are autistic or not it’s always worth taking some time to get to know yourself better and you’re going to learn a lot about autism too!
Related Links
Website
eBook
YouTube
Blog Post
Podcasts

Photo by Johannes Plenio on Unsplash